Rhythm Review: Understanding Cardiac Rhythms in ACLS
Advanced Cardiovascular Life Support (ACLS) is an essential area of Medicine that empowers healthcare professionals to act quickly and efficiently in cardiac emergencies. One of the pillars of the ACLS protocol, following the guidelines of the AHA ACLS and renowned institutions such as Dante Pazzanese, is the recognition of cardiac rhythms. In this educational content, we will explore cardiac arrest rhythms in a didactic, practical way, aligned with what you need to know for the ACLS course, the ACLS exam, or the ACLS test. If you are looking for reliable material, including an ACLS PDF, for your ACLS 2025 certification, this article is for you!
Cardiac Arrest Rhythms: The 4 Essential Categories
In a cardiac arrest, rhythms are organized into four major groups:
- Ventricular Fibrillation (VF)
- Pulseless Ventricular Tachycardia (Pulseless VT)
- Pulseless Electrical Activity (PEA)
- Asystole
These are the pillars of the ACLS algorithm, and understanding them is crucial for anyone working in advanced life support.
Let us detail each one of them in a clear and practical way.
Shockable Rhythms: VF and Pulseless VT
Shockable rhythms are those in which defibrillation is the primary intervention. We are talking about VF and Pulseless VT. But how do you differentiate them? The right question is: "In this rhythm, does the pattern repeat?"
Ventricular Fibrillation (VF)
Here, the answer is no. The tracing on the monitor is chaotic, with no repetitive pattern. The heart is in a state of electrical disarray, unable to pump blood.
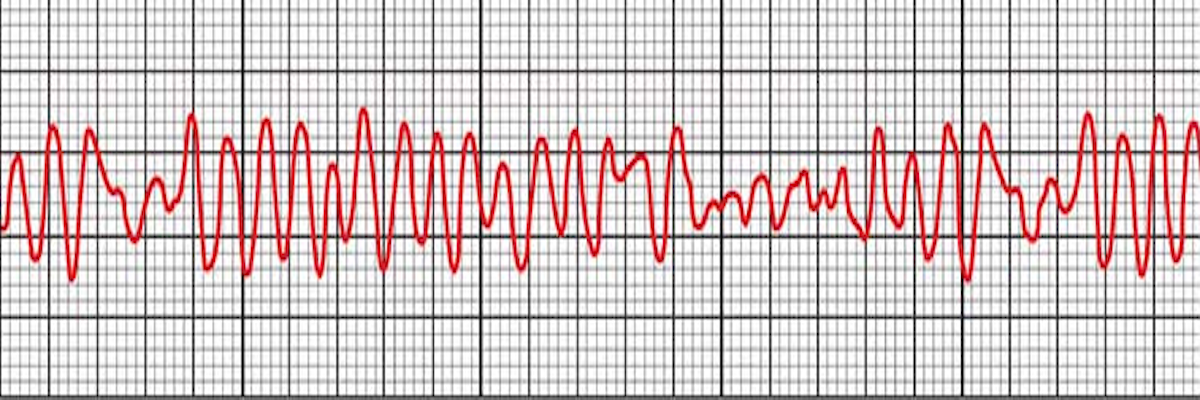
Ventricular Fibrillation -- the pattern does not repeat.
Pulseless Ventricular Tachycardia (Pulseless VT)
Here, the answer is yes. The tracing shows a repetitive pattern, with wide QRS complexes following one another rapidly. It is a ventricular tachycardia that, in a cardiac arrest, does not generate a pulse.
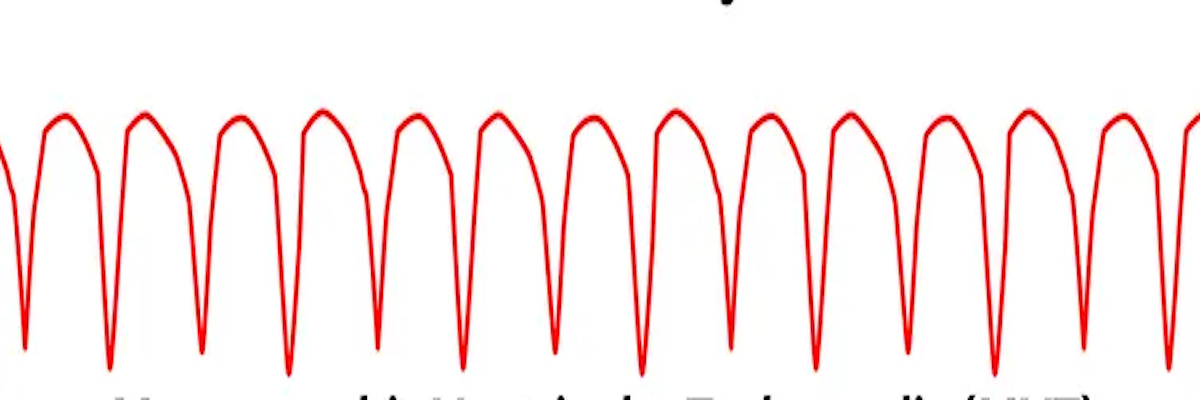
Ventricular Tachycardia -- wide QRS and the pattern repeats.
Bonus: Polymorphic Ventricular Tachycardia and Torsades de Pointes
What about polymorphic VT? It is worth discussing because students always have questions. Ventricular Fibrillation is a subtype of polymorphic VT -- did you know that? Just like the famous Torsades de Pointes, which is also a subtype of polymorphic VT, but has a characteristic undulating pattern, like a "dance" on the monitor. In cardiac arrest, if there is no pulse, all rhythms where the pattern does not repeat are treated as VF, since in VF, the pattern does not repeat.
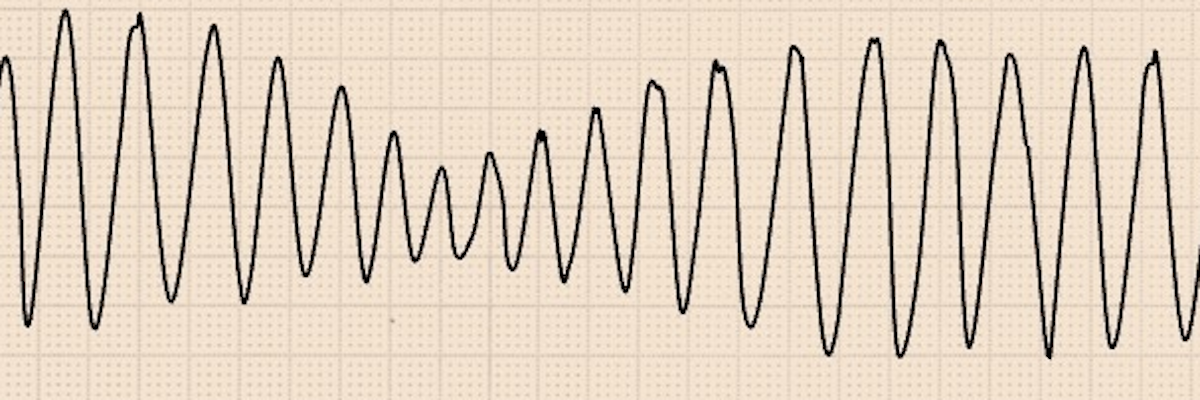
Torsades de Pointes -- the pattern does not repeat. Treat as VF.
The ECG above is a Torsades de Pointes. In a cardiac arrest, what is the question that matters? Does the pattern repeat? No? Then treat as VF and defibrillate the patient.
What is the right question again?
IN THIS RHYTHM, DOES THE PATTERN REPEAT?
- Yes - VT
- No - VF
VF or Pulseless VT? Never get it wrong again with this algorithm
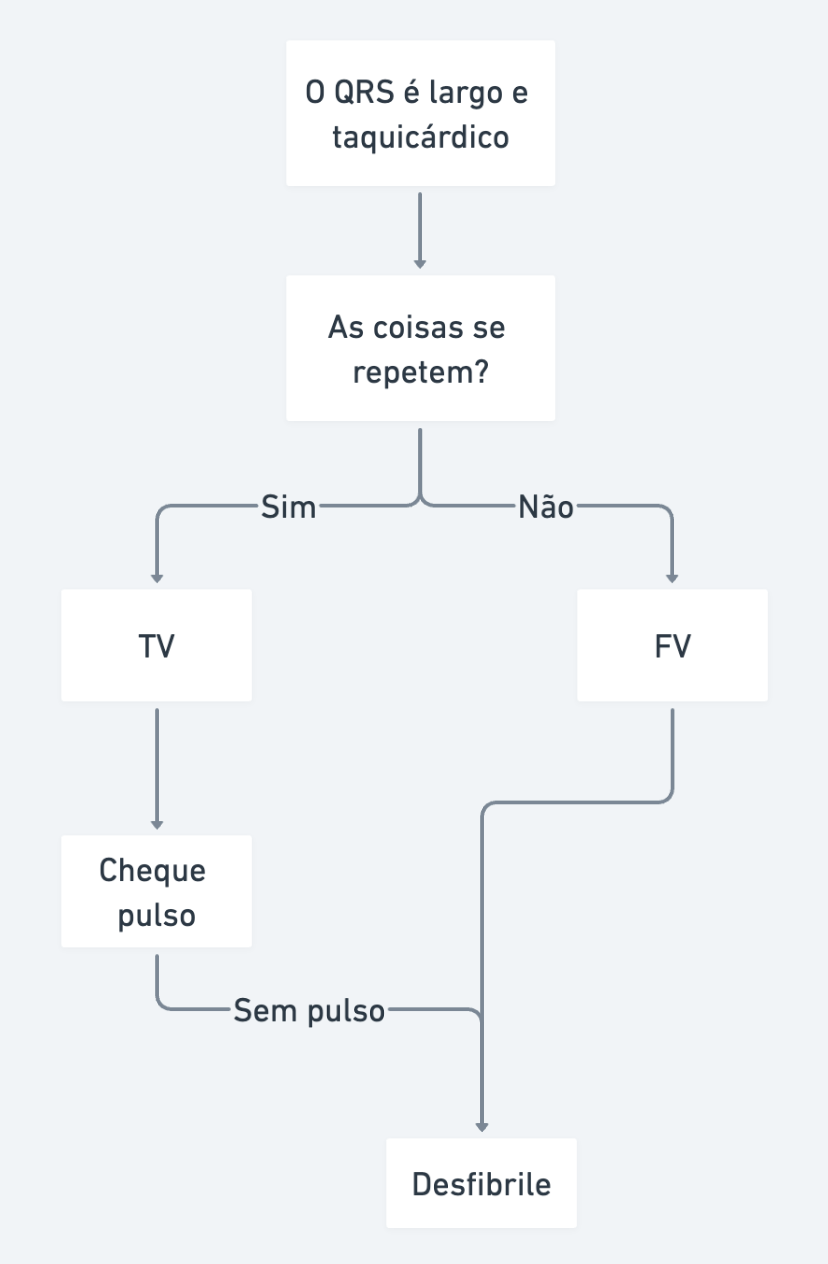
Management
In shockable rhythms, the focus of the ACLS protocol is immediate defibrillation. Just remember: in Ventricular Tachycardia, if there is a pulse, it is not cardiac arrest -- the approach changes. That is why, in the context of cardiac arrest, we call it Pulseless VT.
Non-Shockable Rhythms: PEA and Asystole
Now, let us move on to the rhythms where shock is not the solution: PEA and Asystole.
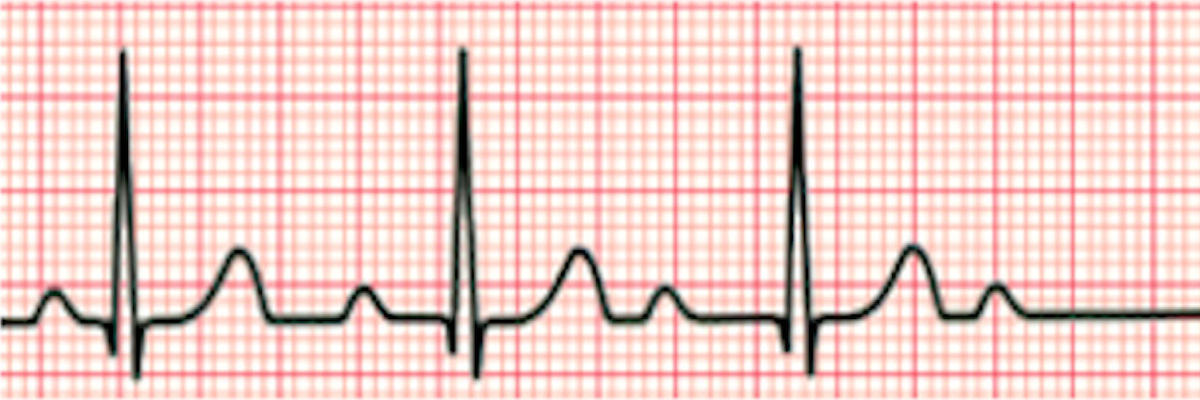
Pulseless Electrical Activity (PEA)
This is the "wildcard" of cardiac arrest rhythms. Any electrical activity on the monitor that is not VF or Pulseless VT, in a patient without a pulse, is classified as PEA. It could be a sinus rhythm, atrial fibrillation (AFib), or even a complete AV block (3rd-degree AV Block) -- if there is no pulse, it is PEA.
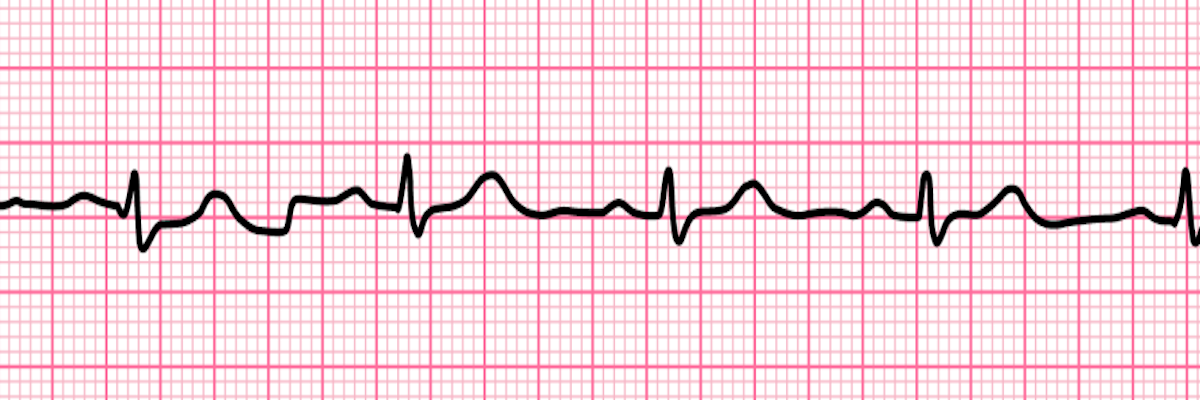
Electrical activity. If the patient is unconscious, they may be in cardiac arrest. Check the pulse -- if absent, it is PEA.
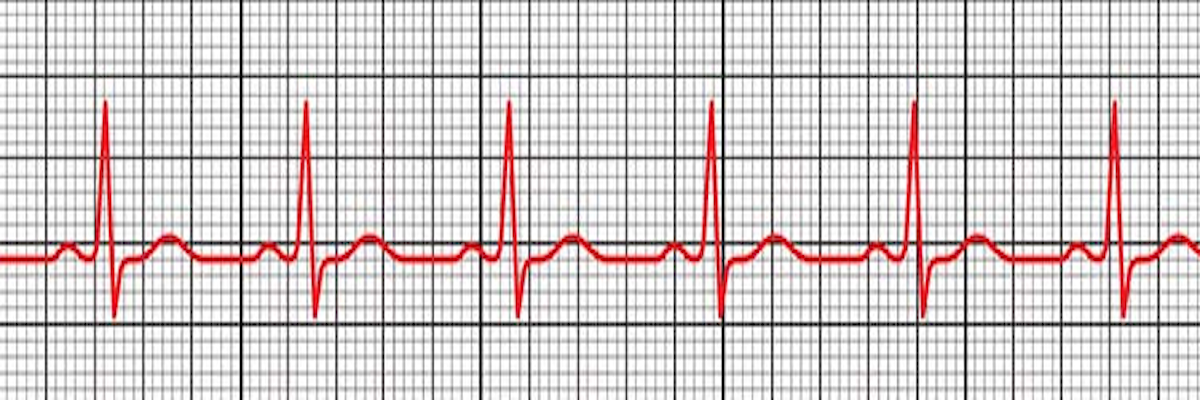
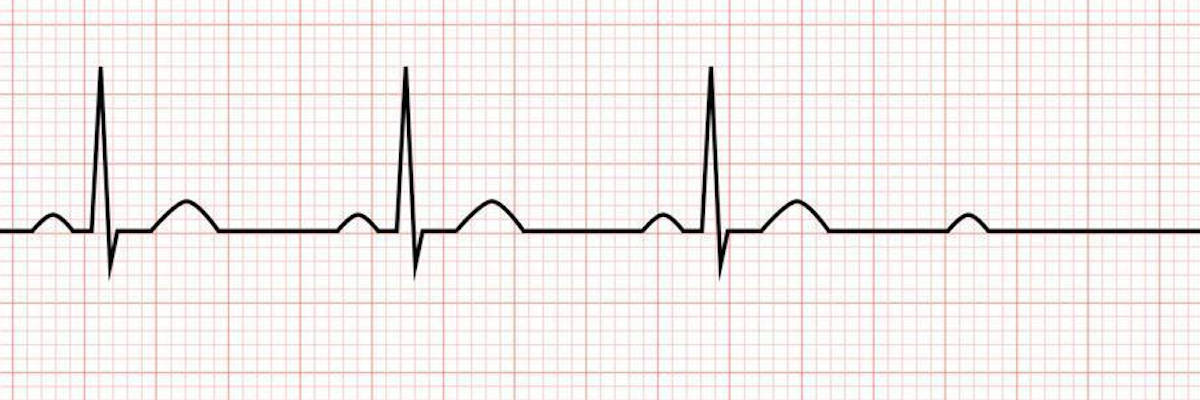
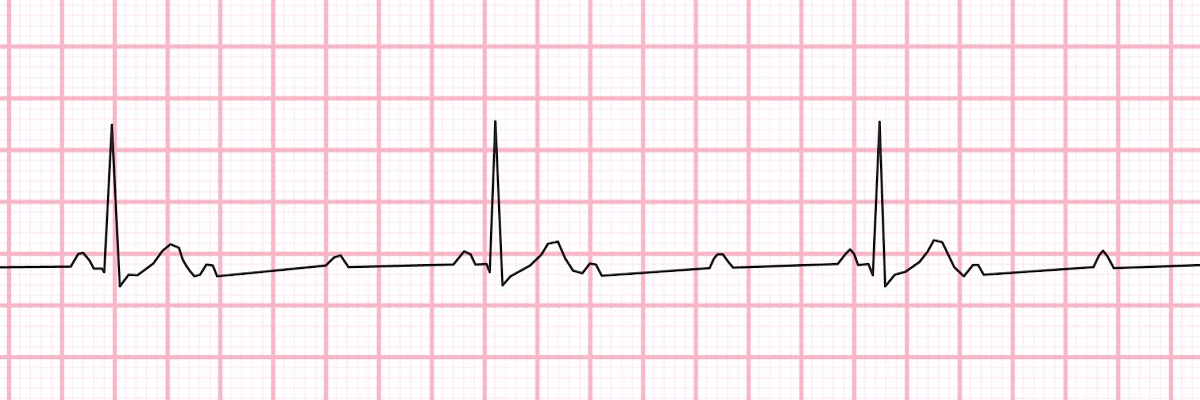
Another example of Pulseless Electrical Activity (PEA).
Both of these rhythms have electrical activity. In a cardiac arrest, if there is no pulse, the rhythm is classified as PEA.
The key here is to check the pulse. Without a pulse, the heart may generate electrical signals but does not pump blood.
Asystole
Pay extra attention here! When you see a flat line on the monitor, initially call it a "flat line" to rule out technical problems (loose cables, gain adjustment, or incorrect lead selection). If the flat line persists, the diagnosis is Asystole.
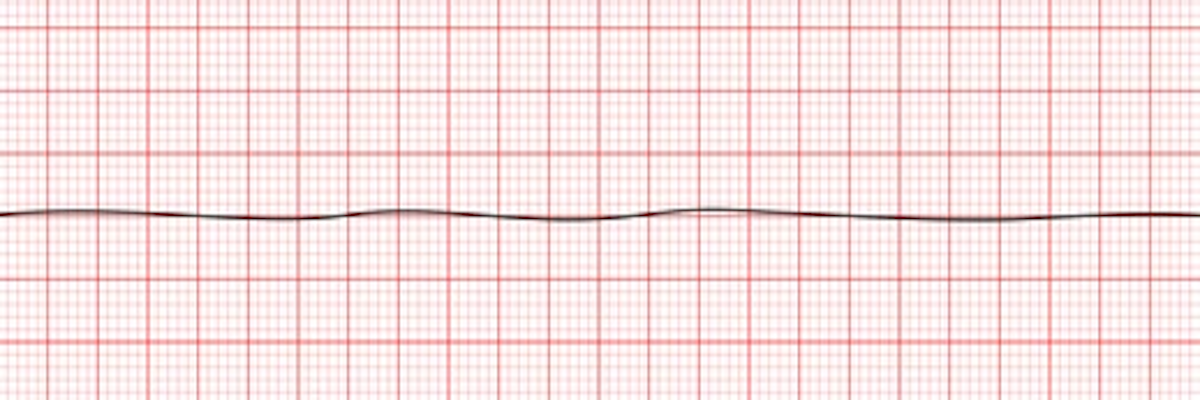
Flat line on the monitor. Only after checking cables, gain settings, and leads can asystole be confirmed.
Practical tip: Asystole is the total absence of electrical activity -- the "silence" of the heart on the monitor.